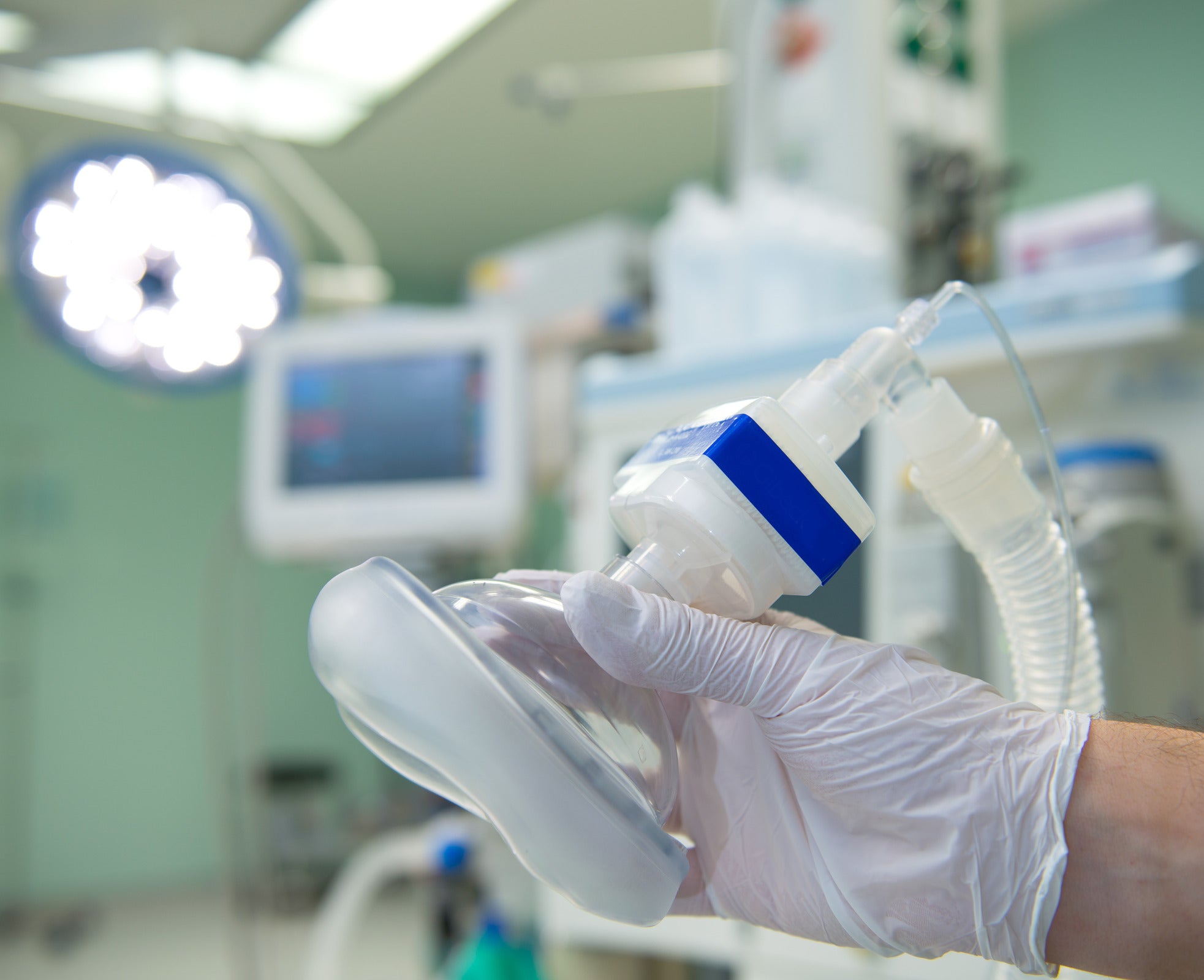
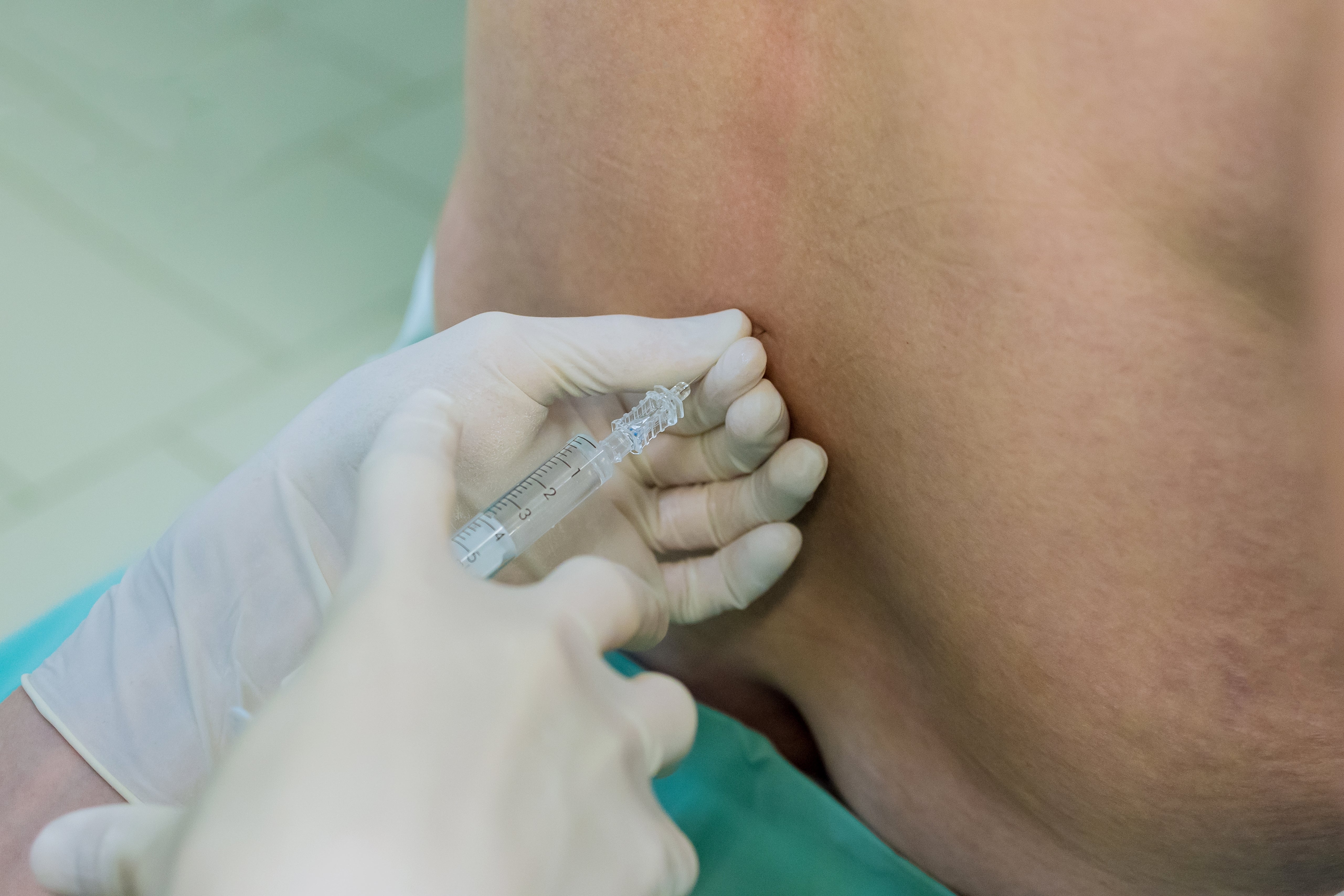
You notice some concerning side effects that make you wonder if it was worth it. This is a common fear for anesthesia patients, especially regarding potential side effects.
The symptoms of a generalanesthetic or regional anesthetic include feeling sick, dizzy, faint, and feeling cold or shivering. It's causing headaches and itchiness. The most common symptoms of this condition are soreness and bruising. Peeing is a problem, and the body aches and pains.
While these effects vary from person to person and depend on different factors, they are essential to understand before deciding on anesthesia.
In this blog post, we will explore several potential side effects of anesthesia, their causes, and how to prepare for them. Our goal is to provide enough information to make an informed decision about your health without causing undue anxiety.
Anesthesia Side Effects: 13 Top Facts

Anesthesia is crucial in modern medicine, enabling patients to undergo surgeries and medical procedures with minimized pain and discomfort. While anesthesia is generally safe and well-tolerated, it's essential to be aware of potential side effects that can arise after its administration. We'll delve into some of the possible side effects of anesthesia, providing valuable insights for patients and caregivers alike.
Nausea and Vomiting
One of the most common side effects following anesthesia is nausea and vomiting. This occurrence can stem from the interaction between anesthesia medications and the body's digestive system. Factors contributing to this side effect include the type of anesthesia used, the duration of the procedure, and individual patient sensitivity.
Sore Throat
Postoperative sore throat is another potential aftermath of anesthesia. This is often attributed to using a breathing tube during surgery, which can cause irritation and discomfort in the throat. Proper hydration and throat lozenges are usually recommended to ease this temporary condition.
Postoperative Delirium
Patients might experience postoperative delirium, characterized by confusion, disorientation, and hallucinations. This can be more common in elderly patients or those with certain preexisting conditions. The exact cause of postoperative delirium isn't fully understood, but factors like the type of surgery, anesthesia medications, and individual vulnerability might contribute.
Muscle Aches
After undergoing anesthesia, it's possible to experience muscle aches and pains. These discomforts are typically the result of the body's positioning during surgery and using muscle relaxants. Mild stretching and gentle movements often help alleviate these temporary discomforts.

Itching
Itchiness is an occasional side effect that some patients might encounter after anesthesia. The exact cause of this itching sensation isn't always clear, but it could be related to the release of histamines in response to the anesthesia drugs.
Chills and Shivering (Hypothermia)
Chills and shivering can occur as a result of anesthesia-induced hypothermia. Anesthesia can interfere with the body's ability to regulate temperature, leading to a drop in body temperature during and after surgery. Warming blankets and other measures are employed to counteract this effect.
Malignant Hyperthermia

Although rare, malignant hyperthermia is a severe reaction to certain anesthesia medications. It causes a rapid increase in body temperature, muscle rigidity, and potentially life-threatening complications. This condition requires immediate medical attention.
Headache
Headaches can develop post-anesthesia due to various factors, including changes in spinal fluid pressure, dehydration, or tension from positioning during surgery. Staying hydrated and using over-the-counter pain relievers under medical guidance can help manage this discomfort.
Minor Back Pain
Patients might experience minor back pain after anesthesia, often related to the body's position on the operating table. This discomfort is usually temporary and can be alleviated with gentle stretching and movement.
Difficulty Urinating
Some individuals encounter difficulty or temporary inability to urinate after anesthesia. This can result from the anesthesia's impact on nerve signals that control bladder function. In most cases, standard urination patterns return once the effects of anesthesia wear off.
Hematoma
A hematoma, or localized blood collection, can form at the injection or anesthetic administration site. While rare, this side effect can lead to pain and swelling. Prompt medical evaluation is necessary if a hematoma is suspected.
Pneumothorax
Anesthesia procedures involving the chest area can lead to a pneumothorax, where air accumulates between the lung and chest wall. This can cause difficulty in breathing and chest pain. Immediate medical attention is crucial to address this issue.
Nerve Damage
Although highly uncommon, nerve damage can occur after anesthesia. This can manifest as numbness, tingling, or weakness in specific body areas. Reporting persistent symptoms to medical professionals for proper evaluation and management is essential.
Side Effects of Anesthesia: Potential Risks and Complications

It's important to acknowledge that, like any medical intervention, it carries certain risks and potential complications. We will delve into these potential risks and complications associated with anesthesia, offering valuable insights for patients, caregivers, and medical professionals.
Allergic Reaction to Anesthetic Medication
An allergic reaction to anesthesia medication is a rare but significant concern. An individual's immune system might react adversely to the components of the anesthesia drugs, leading to an allergic response. It's important to note that an allergy to one type of anesthesia doesn't necessarily imply an allergy to all anesthetics. Factors contributing to allergic reactions include the patient's medical history, allergies, and the specific anesthesia administered.
- Symptoms of an allergic reaction may include skin rash, hives, swelling, difficulty breathing, and in severe cases, anaphylaxis.
- Anesthesia providers carefully review a patient's medical history and allergies to minimize the risk of allergic reactions.
- In an allergic reaction, swift medical intervention is crucial to manage symptoms and ensure patient safety.
Death
While instances of anesthesia-related death are exceedingly rare, it's essential to acknowledge the possibility. Anesthesia involves a delicate balance of medications, and unforeseen complications can arise, potentially leading to severe outcomes. It's essential to emphasize that most anesthesia procedures are conducted successfully without life-threatening incidents.
- The risk of anesthesia-related death is significantly low, especially when administered by experienced anesthesia professionals.
- Preoperative evaluations and thorough patient assessments help identify and mitigate potential risk factors that could contribute to adverse outcomes.
- Anesthesia providers are trained to monitor patients closely throughout procedures to address emergent situations promptly.

Permanent Nerve Damage
Permanent nerve damage is an infrequent yet severe complication associated with anesthesia. Nerve damage can occur due to various factors, including the patient's positioning during surgery, the administration of anesthesia, or pressure on nerves during the procedure.
- Symptoms of nerve damage may include numbness, tingling, muscle weakness, or loss of sensation in specific body areas.
- Anesthesia providers take precautions to minimize nerve damage risks, such as careful positioning and constant monitoring during surgery.
- If nerve damage is suspected post-surgery, diagnostic tests and consultations with medical specialists are typically conducted to assess and manage the situation.
Anesthesia Side Effects: Understanding Different Types
As medical science advances, so does our understanding and application of anesthesia, a critical tool in ensuring patient comfort and safety during medical procedures. Anesthesia comes in various forms, each tailored to specific situations and needs. We will delve into the different types of anesthesia, shedding light on how each work and their unique benefits.
Local anesthesia

Local anesthesia is a localized numbing technique that blocks sensation in a specific body area. It's commonly employed for minor surgical or medical procedures.
How it works:
- Local anesthetic drugs are injected directly into or around the area requiring treatment.
- These drugs temporarily block nerve signals in the vicinity, preventing pain signals from reaching the brain.
- Local anesthesia is often used for dental work, suturing, and skin biopsies.
Sedation
Sedation involves using medication to induce a relaxed, drowsy state, reducing anxiety and discomfort during procedures that don't necessarily require complete unconsciousness.
How it works:
- Sedative medications, such as benzodiazepines or certain opioids, are administered orally, intravenously, or inhaled.
- Patients remain conscious but are in deep relaxation, often with limited memory of the procedure.
- Sedation is commonly used for minor surgeries, endoscopic procedures, and interventions where patient cooperation is necessary.
Regional Anesthesia
Regional anesthesia involves numbing a more significant portion of the body, typically a limb or a section, by targeting specific nerves. This technique relieves pain and allows the patient to remain awake and alert.
How it works:
- Anesthetic drugs are injected near nerves that supply sensation to a specific region, effectively blocking nerve signals.
- Regional anesthesia can be subdivided into nerve blocks, epidurals, and spinal, depending on the targeted area.
- This type of anesthesia is often chosen for orthopedic surgeries, childbirth, and postoperative pain management.
General Anesthesia
General anesthesia is the most comprehensive form of anesthesia, inducing a controlled state of unconsciousness and a complete lack of sensation. It's utilized for complex surgeries and procedures.
How it works:
- General anesthetic medications are administered intravenously or inhaled to induce a state of unconsciousness.
- The patient is closely monitored throughout the procedure, carefully controlling and adjusting vital signs.
- General anesthesia ensures the patient is entirely unaware and pain-free during the surgery, allowing the medical team to perform intricate procedures.
Anesthesia Side Effects: Preparation Methods
Proper preparation is a cornerstone of a successful anesthesia experience, promoting patient safety, comfort, and effective medical interventions. We'll delve into the crucial aspects of preparing for anesthesia, offering insights into how patients should optimize their anesthesia encounters:
Medical Evaluation

Before anesthesia, a comprehensive medical evaluation is essential to assess a patient's health status, identify potential risk factors, and tailor the anesthesia plan accordingly.
Key Points:
- Anesthesia providers will review your medical history, including preexisting conditions, allergies, and current medications.
- A physical examination may assess your overall health and vital signs.
- Preoperative tests, such as blood work and imaging studies, might be ordered to ensure your body is ready for anesthesia.
Dietary Guidelines
The adhesion to fasting guidelines is crucial to prevent complications during anesthesia and surgery. Proper fasting helps reduce the risk of aspiration (inhaling stomach contents) and related respiratory issues.
Key Points:
- Patients are typically advised not to eat or drink for a specified duration before the procedure, often starting at midnight.
- Based on your anesthesia provider's recommendations, clear liquids might be allowed up to a few hours before the procedure.
- Following fasting guidelines helps ensure an empty stomach, reducing the risk of aspiration during anesthesia.
Medication Restrictions
Certain medications can interact with anesthesia drugs or impact the anesthesia process. It's essential to communicate all medicines, supplements, and herbal remedies you are taking to your anesthesia provider.
Key Points:
- Some medications need to be temporarily paused or adjusted before the procedure.
- Inform your anesthesia provide about any blood-thinning medications, as they can affect bleeding during surgery.
- Following your anesthesia team's medication instructions is crucial to prevent potential complications.
Arrangements for After Surgery
The preparation for postoperative care ensures a smooth transition from the surgical facility to your recovery environment.
Key Points:
- Arrange for a responsible adult to accompany you and drive you home after the procedure, especially if you've received sedation or general anesthesia.
- Ensure you have a comfortable and safe recovery area at home with the necessary supplies, medications, and contact information for your healthcare providers.
- Understand any postoperative instructions, including restrictions on activities and follow-up appointments.
Anesthesia Side Effects: Administration
The administration of anesthesia is a critical phase in any medical procedure, requiring precision, expertise, and careful monitoring to guarantee patient safety and comfort. We'll delve into the vital components of administering anesthesia, shedding light on the roles of anesthesia providers, monitoring protocols, duration considerations, and the recovery process.
The Role of the Anesthesiologist

Anesthesia administration involves a team of highly skilled professionals, with the anesthesiologist at the forefront, responsible for ensuring the patient's well-being throughout the procedure.
Key Points:
- An anesthesiologist is a medical doctor trained in anesthesia and perioperative care.
- The anesthesiologist assesses the patient's medical history, selects the appropriate anesthesia type, and administers anesthesia medications.
- They continually monitor the patient's vital signs, adjust anesthesia levels as needed, and manage any emergent situations that may arise.
Monitoring During Anesthesia
Continuous monitoring during anesthesia is essential to detect any changes in the patient's condition and respond promptly to ensure their safety.
Key Points:
- Patients are monitored during anesthesia for vital signs such as heart rate, blood pressure, oxygen saturation, and respiratory rate.
- Monitoring devices and equipment provide real-time data to the anesthesia team, such as electrocardiograms (ECGs), pulse oximeters, and blood pressure cuffs.
- Anesthesia providers maintain vigilant oversight throughout the procedure to adjust anesthesia levels and respond to deviations from normal parameters.

Duration of Anesthesia
The duration of anesthesia varies depending on the procedure and anesthesia type. Anesthesia providers strive to maintain the optimal balance between patient comfort and safety.
Key Points:
- Local anesthesia and sedation are typically shorter in duration and often employed for minor procedures.
- Regional and general anesthesia is used for longer surgeries and procedures requiring a controlled state of unconsciousness.
- Anesthesia providers carefully manage anesthesia levels to ensure patients remain comfortable while minimizing the risk of prolonged unconsciousness.
Recovery from Anesthesia
The recovery phase after anesthesia is crucial for ensuring patients regain consciousness, stabilize vital signs, and transition smoothly to a postoperative environment.
Key Points:
- Anesthesia providers carefully titrate the anesthesia medications as the procedure concludes, allowing patients to awaken gradually.
- Patients are monitored in a post-anesthesia care unit (PACU) until they are fully conscious and have stable vital signs.
- Recovery times vary depending on the anesthesia type, procedure complexity, and individual patient factors.
Conclusion
While anesthesia is an essential part of modern medicine, it's important to understand its significant risks. The anesthesia experience varies from person to person, but being aware of potential side effects is crucial.
Doing thorough research, discussing your medical history, and asking your anesthesiologist questions can ensure a smoother experience and reduce the risks of complications.
We hope this post has given you enough knowledge to make informed decisions and have a successful surgery. Remember, your health is paramount, so don't hesitate to ask questions or talk to your medical provider. Stay informed, stay safe, and take care of yourself.
![13 Top Anesthesia Side Effects & Potential Risks [covered]](http://drnumb.com/cdn/shop/articles/shutterstock_1781191736_1.jpg?v=1693284851&width=1100)