Spinal anesthesia is commonly used for pain relief in surgeries, especially in the lower abdomen, pelvis, and lower extremities. It works by injecting anesthetics and painkillers into the subarachnoid space near the spinal cord to numb nerves, providing a pain-free surgical experience.
The midline approach is commonly used during a spinal anesthetic procedure, and several layers of anatomy are traversed before reaching the subarachnoid space. These include the skin, subcutaneous fat, supraspinous ligament, interspinous ligament, ligamentum flavum, dura mater, subdural space, arachnoid mater, and the subarachnoid space itself.
While spinal anesthesia carries some risks, such as headache, nerve damage, and infection, it is considered a safe and effective option for many surgical procedures.
In this blog post, we will explore the ins and outs of spinal anesthesia, including how it is performed, what to expect during the procedure, and its potential benefits and drawbacks.
Spinal Anesthetic Procedure: 6 Techniques

Spinal anesthetics relieve pain and temporary paralysis in the affected area by injecting anesthetics into the cerebrospinal fluid, usually in the lumbar region. Generally, it is used in lower body surgeries, like cesarean sections and hip replacements.
Patient Positioning
Proper patient positioning is crucial for a successful spinal anesthetic procedure. Here are some important considerations and steps to ensure optimal patient positioning.
Sitting Position for Hyperbaric Solution:
- The sitting position is chosen when using a hyperbaric solution for spinal anesthesia.
- This position assists in effectively distributing the anesthetic solution within the spinal canal.
Lateral Decubitus Options:
- Both left, and right lateral decubitus positions are suitable alternatives.
- These positions are particularly useful for patients who might not be comfortable in a sitting position.
Access Site Identification:
- Once the patient is positioned appropriately, the healthcare provider identifies the access site by palpation.
- Palpation helps locate the optimal entry point on the patient's back for accurate needle insertion.
Importance of Positioning:
- Patient positioning plays a crucial role in the success of spinal anesthesia.
- Proper positioning enhances access to the spinal canal and aids in precisely administering the anesthetic solution.
The spinal anesthetic procedure can be performed smoothly and safely by following these steps and ensuring the patient is in the proper position. It is important to note that trained medical professionals should only do proper patient positioning.

Sterilization of The Area
During a spinal anesthetic procedure, proper sterilization of the area is essential to ensure patient safety and prevent the risk of infection. This step is crucial as contamination of the injection site may lead to serious complications such as meningitis, abscess formation, or nerve damage.
This section will discuss the importance of sterilization, the steps involved in the process, and the different techniques used in spinal anesthesia.
Autoclaving Local Anesthetics:
- Local anesthetics frequently employed in spinal procedures can be sterilized through autoclaving.
- Autoclaving involves subjecting the anesthetics to high heat and pressure to eliminate microbes and ensure a sterile environment.
Optimal Sterilization Conditions:
- The local anesthetics are autoclaved at specific conditions: 30 minutes at temperatures ranging from 255 to 260°F (124 to 127°C).
- The pressure maintained during autoclaving is 18 to 20 lb. (1.22 to 1.36 atmospheres above ambient pressure).
Preservation of Potency:
- The crucial aspect of this sterilization process is that the local anesthetics maintain their potency even after autoclaving.
- This means that anesthetics can effectively relieve pain during the spinal procedure.
Enhanced Infection Control:
- Autoclaving local anesthetics enhances infection control by ensuring that the substances administered to patients are completely sterile.
- Sterilization of the anesthetics minimizes the risk of introducing contaminants and pathogens into the patient's body during the procedure.
Selection Of Anesthesia

One of the critical aspects of carrying out a spinal anesthetic procedure is selecting the most appropriate anesthesia for the patient. The anesthesia chosen will depend on various factors, such as the patient's health status, the type and duration of the surgery, and the healthcare provider's preferences. This section will discuss the different anesthesia and how they are selected.
Types of Anesthesia
Anesthesia renders a patient unconscious and painless during surgery or other medical procedures. General anesthesia, regional anesthesia, local anesthesia, and sedation anesthesia are the four main types. Anesthesia is determined by surgery type, medical history, and individual preferences.
General Anesthesia: General anesthesia is a type of anesthesia that renders the patient unconscious. An anesthesiologist or nurse anesthetist administers it. The patient's breathing, heart rate, and blood pressure will be monitored closely during general anesthesia. This type of anesthesia is typically used in major organ surgeries or longer procedures.
Local Anesthesia: Local anesthesia is administered to numb a particular body area. It is often used in minor surgical procedures and dental work. It is not usually used for surgeries that require more extensive anesthesia.
Regional Anesthesia: Regional anesthesia is used to numb a larger portion of the body. Such anesthesia is usually required for arms, legs, or midsection procedures. There are two main types of regional anesthesia:
- Epidural anesthesia: Administered in the epidural space, a small space between the spinal cord and the vertebrae.
- Spinal anesthesia: Administered directly into the fluid surrounding the spinal cord.
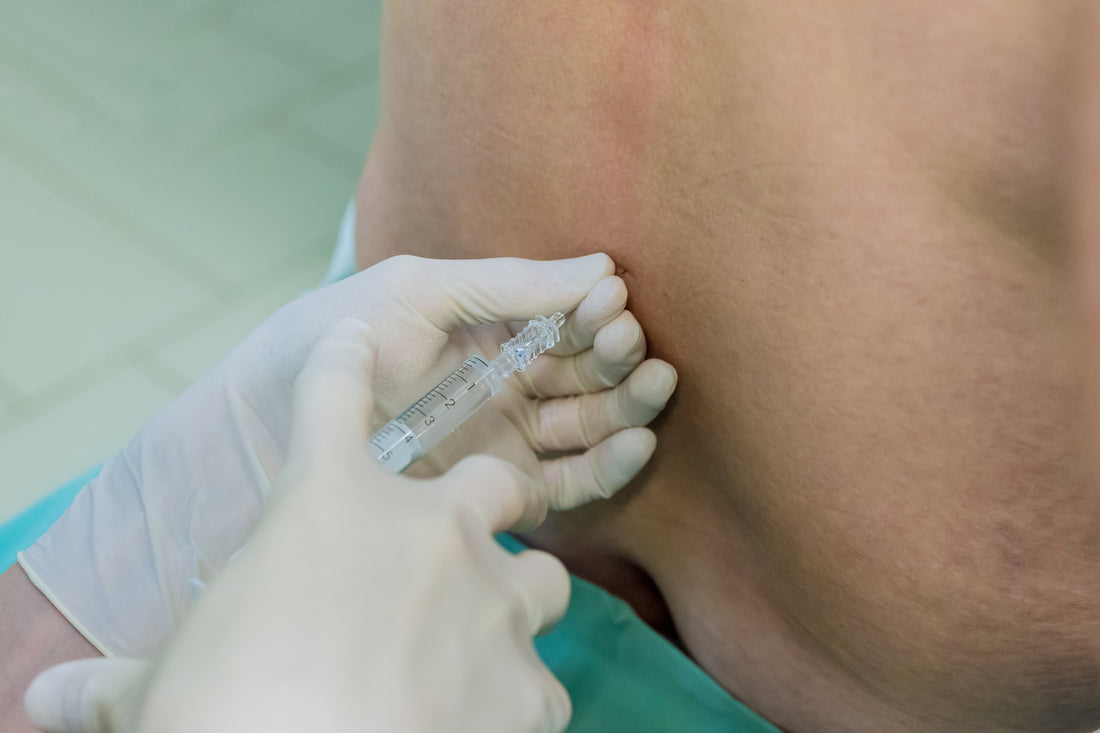
Needle Insertion
The precise and carefully executed step of needle insertion is a pivotal moment in the spinal anesthetic procedure. This stage sets the foundation for successful anesthesia administration and plays a crucial role in ensuring patient comfort and safety.
- Needle Placement: The procedure involves inserting a needle between the lumbar vertebrae, specifically through the dura mater, a protective spinal cord membrane.
- Anesthetic Medication: The needle insertion allows for the precise delivery of anesthetic medication into the subarachnoid space, which acts on nerve roots and relieves pain.
- Anatomy Focus: The placement considers the anatomy of the bony spine and vertebrae. This ensures accuracy and minimizes the risk of complications during the needle insertion process.
- Injection Site:The target site for needle insertion is carefully chosen to optimize access to the subarachnoid space, promoting effective anesthetic distribution for the intended procedure.

Injection of Local Anesthesia
The spinal anesthetic procedure involves injecting a local anesthetic into the cerebrospinal fluid surrounding the spinal cord. This results in a temporary loss of sensation and muscle function in the lower half of the body. The injection of local anesthesia is a critical component of the procedure, as it numbs the nerves that transmit pain signals from the lower body to the brain.
- Neuraxial Anesthesia Technique: Spinal anesthesia involves a neuraxial approach where a local anesthetic is injected into the cerebrospinal fluid (CSF) within the lumbar spine.
- Targeted Nerve Anesthesia: The injection aims to anesthetize the nerves exiting the spinal cord, providing localized and effective pain relief for specific regions of the body.
- Precise Lumbar Location: The injection is carefully administered into the lumbar region of the spine, a strategic location that allows for optimal distribution of the local anesthetic throughout the CSF.
- Onset and Duration: The local anesthetic injection results in rapid onset of anesthesia, leading to numbness and pain relief in the targeted area. The duration of anesthesia varies based on the type and amount of local anesthetic used, as well as individual patient factors.
Adequate Pain Relief in Spinal Anesthetic
Providing adequate pain relief is crucial for the patient's comfort and safety during surgical procedures. Confirmation of adequate pain relief in a spinal anesthetic procedure involves several steps to minimize the patient's pain. Here are some key points to consider:
- Purpose of Confirmation: After administering an epidural or spinal block injection, the healthcare provider ensures the patient's pain relief is adequate and on target, reflecting the successful implementation of the anesthesia.
- Assessment of Sensation: The confirmation process involves assessing the patient's sensory responses in the targeted area. This can include asking the patient about sensations or testing their response to touch, pressure, or temperature.
- Real-Time Feedback: Healthcare providers may request immediate feedback from the patient to gauge the effectiveness of the injected anesthesia. This interaction helps make any necessary adjustments if the desired level of pain relief has yet to be achieved.
- Adjustments if Needed: If the patient reports persistent pain or discomfort, healthcare providers may consider further anesthesia adjustments or interventions to optimize pain relief, ensuring the patient's comfort during the procedure or surgery.

The patient's comfort and safety depend on the pain relief level provided during spinal anesthesia procedures. Monitoring vital signs, pain assessment, administering additional medications, communicating clearly with the patient, and evaluating pain relief.
Layer Traverse Of Spinal Anesthetic Procedure
During a spinal anesthetic procedure, the needle must traverse through several layers before reaching the target area, the subarachnoid space. Each layer presents unique challenges and requires a particular technique to minimize the risk of complications.
Skin
The skin is the first layer the needle penetrates during a spinal anesthetic procedure. Adequate sterile technique must be observed at all times to prevent infection.
- Local Anesthetic Infiltration: A small amount (approximately 1 ml) of 1% lidocaine, a local anesthetic, is injected into the skin to numb the needle's insertion area.
- Wheal Creation: The injection forms a small raised area known as a "wheel," ensuring that the skin and underlying tissue are numbed for the procedure.
- Access Site Choice: The wheel is created at either a midline or paramedian location, with the midline approach involving a straight-line shot toward the intrathecal space for the spinal anesthesia procedure.
Subcutaneous Fat
The subcutaneous fat layer is thick in some patients, making it challenging to visualize the underlying structures during the procedure. The needle must be inserted at the correct angle to avoid hitting any bone structure.
- Location: Subcutaneous fat is just beneath the skin and above the muscles.
- Role: It is a protective cushioning layer and an energy reserve for the body.
- In Midline Approach: During the midline approach for a spinal anesthetic procedure, the spinal needle passes through the subcutaneous fat layer after the skin, following the trajectory towards the intrathecal space.
Supraspinous Ligament
The supraspinous ligament is a dense fibrous tissue that connects the spinous processes. The first ligament the needle crosses in the spinal canal, and must be traversed with care to avoid an accidental needle puncture.
- Supraspinous Ligament: The supraspinous ligament, a fibrous band located along the posterior aspect of the spine, is part of the pathway for needle insertion during spinal anesthesia. The needle penetrates the subcutaneous tissue, interspinous ligaments, and skin, facilitating progression toward the subarachnoid space.
- Key Role in Pathway: The supraspinous ligament's inclusion in the needle's path is vital for accurate needle placement during spinal anesthesia. It adds structural support to the spine and marks a significant anatomical landmark as the needle advances toward its destination in the subarachnoid space, contributing to the precision and safety of the procedure.
Interspinous Ligament

The interspinous ligament is the second ligament the needle passes through in a spinal anesthetic procedure. It is a thin and easily torn membrane and should be cautiously approached.
- Interspinous Ligament Role: During the spinal anesthetic procedure, the interspinous ligament is an initial point of reference, guiding the introducer needle's midline approach along the desired needle path.
- Needle Pathway Foundation: It acts as a foundation for the subsequent insertion of the spinal needle, ensuring a precise and well-aligned trajectory for accurate anesthesia administration.
Ligamentum Flavum
Ligamentum flavum connects adjacent vertebrae's lamina and is a thick, elastic tissue. It provides resistance to the needle, requiring considerable force to pass through it.
- Ligamentum Flavum Role: This structure within the spinal canal is crucial for procedures involving the lower extremities, perineum, pelvic girdle, or lower abdomen. It must be carefully traversed or penetrated during needle insertion to reach the subarachnoid space.
- General Anesthesia for Lumbar Spine Surgery: General anesthesia (GA) is the preferred choice for lumbar spine surgery, primarily due to the complexity and invasiveness of such procedures. While spinal anesthesia may be used for diagnostic or less-invasive lumbar procedures, the decision between GA and spinal anesthesia is made based on the specific surgery's requirements and patient factors.
Dura Mater
The dura mater is a tough, dense membrane covering the spinal cord. Special care must be taken when inserting the needle through this layer to prevent it from puncturing the underlying nerves.
- Dura Mater and Spinal Anesthesia: The dura mater is a protective membrane surrounding the spinal cord and cerebrospinal fluid. During a spinal anesthetic procedure, a needle is carefully inserted through the dura mater to access the subarachnoid space to administer anesthetic medication.
- Needle Penetration for Medication: A needle is inserted between the lumbar vertebrae and through the dura mater in spinal anesthesia. The precise placement of the anesthetic medication allows the provider to relieve pain effectively in the subarachnoid space.
Subdural Space
The subdural space is a potential space between the dura mater and the arachnoid mater. It is crucial to avoid puncturing this space since it contains delicate blood vessels.
- Subdural Space in Spinal Anesthesia: The subdural space refers to the potential area between the dura mater (outermost protective layer of the spinal cord) and the arachnoid mater (middle layer) within the spinal canal.
- Impact on Sensory Block: Injecting local anesthetic into the subdural space during a spinal anesthetic procedure can cause a profound sensory block, occasionally affecting cranial nerves because of the extension of this space into the skull.
Subarachnoid Space

The needle reaches the subarachnoid space to inject an anesthetic solution. Careful care is needed to avoid unwanted complications and nerve injuries.
- Intrathecal Location: The subarachnoid space is the specific location within the spine where spinal anesthesia is administered, involving local anesthetic injection into this space.
- Cerebrospinal Fluid Reservoir: It is a sterile area filled with cerebrospinal fluid (CSF), a clear fluid surrounding and protecting the brain and spinal cord, providing a cushioning effect.
Prevent complications and nerve injury by treating each layer carefully during spinal anesthesia. The structure and function of each layer can aid in proper assessment and technique.
Pre-Procedure Preparation
Pre-procedure preparation for spinal anesthetics includes obtaining the patient's consent and reviewing their medical history. During the procedure, administering pre-emptive analgesia will reduce the patient's discomfort.

Medical evaluation
An extensive medical evaluation is necessary before undergoing a spinal anesthetic. We ensure the patient is healthy and a good candidate during this evaluation.
Medical evaluations are crucial before spinal anesthetics:
- Identification of Medical History: As part of a medical evaluation, a physician will review the patient's medical history to identify any underlying conditions. This information is crucial in determining the patient's procedure eligibility and identifying potential risks.
- Recognition of Allergies and Sensitivities: Patients may be allergic to certain medications or anesthetics. A medical evaluation helps identify allergies and sensitivities, allowing the physician to choose an appropriate anesthetic.
- Evaluation of Medication Use: Certain medications may interfere with the spinal anesthetic procedure. During the medical evaluation, the physician will review the patient's medication regimen to identify any drugs that may need to be discontinued or changed before the procedure.
- Assessment of Current Health Status: A medical evaluation will also assess the patient's health status. This evaluation includes physical exams and possibly laboratory tests to determine any current health problems that may affect the spinal anesthetic procedure.
- Reducing Risks: The medical evaluation aims to reduce the risks of complications during the spinal anesthetic procedure. By identifying potential issues beforehand, the physician can take precautions to minimize risks during the procedure.
The Importance of Medication Review

A meticulous review of a patient's medication history is essential in a spinal anesthetic procedure to ensure patient safety and minimize the risk of complications. As a medical professional, here are some crucial details you should consider:
- Some medications can increase bleeding: Medications like aspirin, nonsteroidal anti-inflammatory drugs, and blood-thinning medication can increase the risk of bleeding during the procedure. Therefore, these medications should be disclosed to assess the risk of intraoperative bleeding.
- Pain medications: Analgesics like opioids can interfere with the efficacy of the anesthetic, making them difficult to monitor and regulate.
- Blood pressure medicine: Some medications used to regulate blood pressure may interact adversely with the anesthetic medication, leading to an unsafe drop in blood pressure, a vital consideration for the anesthesiologist.
- Diabetic medication: Proper management of blood glucose levels is crucial for diabetic patients. Before the procedure, medical professionals must assess the patient's diabetic management plan and adjust medication doses accordingly.
Consent Form
A consent form is a legal document to sign before undergoing spinal anesthesia. There are risks and benefits, alternatives to the procedure, and possible side effects. Consent forms inform you about the procedure and its potential outcomes. A spinal anesthetic procedure requires preparation just as much as consent. Here are some things to consider:
- Fasting: Your healthcare provider will probably advise you not to eat or drink anything for at least 6-8 hours before the procedure. This is to prevent the risk of aspiration, where food or liquid enters the lungs during the anesthesia.
- Medical History: Your healthcare provider will ask for your medical history and information about any medications or supplements you are currently taking. It is important, to be honest and provide complete information about your health status, as this can affect the anesthesia's effectiveness.
- Dealing with anxiety: You might feel anxious or nervous before the procedure. Speak to your healthcare provider about any concerns you have, and they will be able to provide information and advice to alleviate your worries.
- Know What to Expect: Talk to your healthcare provider about what to expect during the procedure. Understanding the procedure process can help ease anxiety and ensure you're fully prepared.
Spinal anesthetic procedures require consent forms and proper preparation before being performed. Keep your medical history honest with your healthcare provider to decrease risks and increase success rates.
Post-Procedure Considerations
Patient recovery continues after spinal anesthetic procedures with diligent post-procedure care and attention. This phase is essential for ensuring the patient's well-being, minimizing complications, and preparing them for a return to normal activities.
Monitoring Of Vital Signs

- Regular monitoring of vital signs, including blood pressure, heart rate, respiratory rate, and oxygen saturation, is essential to promptly detect any changes or complications.
- Patients are often observed for a designated period in a recovery area to assess their stability after the procedure.
- Close observation allows for the early identification of any adverse reactions or unexpected developments.
Management Of Adverse Reactions
- Close monitoring for potential adverse reactions, such as allergic responses, hypotension (low blood pressure), or changes in neurological status, is crucial.
- Healthcare providers are equipped to respond promptly to any emergent situations.
- Rapid and appropriate intervention strategies are employed in the event of adverse reactions.
- Medications, fluid management, or other interventions may be utilized to stabilize the patient's condition.
Pain Management Post-Procedure
- Patients are regularly assessed for post-procedure pain levels using standardized pain scales.
- Effective pain management enhances patient comfort and overall satisfaction.
- Oral and intravenous pain relief medications are administered as needed based on the patient's pain intensity and medical history.
- Optimal pain management balances alleviating discomfort and allowing patients to regain mobility gradually.
- Early mobilization can aid in preventing complications such as blood clots.
Hospital Discharge Process
- Patients are discharged once they meet specific criteria, including stable vital signs, adequate pain control, and the resolution of any immediate post-procedure effects.
- Discharged patients receive thorough instructions on post-procedure care, pain management, and potential warning signs requiring medical attention.
- Healthcare providers schedule follow-up appointments to monitor the patient's progress and prevent complications.
- Patients are provided with written instructions for self-care at home, including medication schedules, wound care, and activity restrictions.
- Patients are given contact information to reach healthcare providers in case of questions, concerns, or unexpected developments.
Post-procedure phases of spinal anesthetic procedures are as critical as the preceding stages. Managing vital signs, adverse reactions, addressing pain, and guiding patients through the hospital discharge contribute to successful patient recovery. Providers uphold their commitment to patient well-being by meticulously observing, responding to, and educating patients.
Risks and Complications
There are inherent risks and complications associated with spinal anesthesia. To ensure patient safety and informed decisions, healthcare providers assess and manage risks comprehensively. As a patient or healthcare provider, you should be aware of the various risks associated with spinal anesthesia, from minor to major.
Minor Risks

- Headache: A post-procedure headache is frequent, typically caused by cerebrospinal fluid leakage from the needle insertion site. It usually resolves within a few days with rest and hydration.
- Nausea and Vomiting: These symptoms may arise due to the effects of anesthesia, medications, or changes in blood pressure.
- Shivering and Chills: The body's temperature regulation can be temporarily affected, leading to shivering and chills.
- Bruising or Bleeding: There may be mild bruising or minimal bleeding at the needle insertion site.
Major Risks
Serious but Rare Major Risks Include:
- Infection: Infection at the needle insertion site or in the spinal canal is a rare but serious complication.
- Nerve Damage: The needle's accidental contact with nerves can cause temporary or, in rare cases, permanent nerve damage.
- Bleeding: Excessive bleeding around the spinal cord, leading to compression, can be a serious complication.
- Hypotension (Low Blood Pressure): A sudden drop in blood pressure may lead to dizziness, fainting, or even fainting.
- Allergic Reactions: Rare allergic reactions to local anesthetics or other medications can occur.

Long-Term Complications
- Back Pain: Some patients may experience localized back pain at the needle insertion site that persists beyond the immediate post-procedure period.
- Nerve Injury: In rare instances, nerve injury resulting from the procedure can lead to chronic pain, weakness, or altered sensations.
- Arachnoiditis: Inflammation of the arachnoid membrane can cause chronic pain and neurological symptoms.
- Cerebrospinal Fluid Leakage: Prolonged cerebrospinal fluid leakage can lead to headaches and other complications.
Maintaining open communication and promptly addressing concerns helps patients and healthcare providers navigate potential risks and complications.
Conclusion:
In summary, spinal anesthesia is a valuable tool in modern medicine that has revolutionized complex surgeries. It carries less risk of complications than traditional general anesthesia and allows patients to recover faster. As with any medical procedure, spinal anesthesia has some risks, such as headaches and nerve damage, which should be appropriately discussed with the anesthesiologist before the procedure.
Overall, the benefits of spinal anesthesia far outweigh the risks, and it is an excellent option for those looking for a pain-free surgery or childbirth experience. So, if you are planning for any surgical procedure or childbirth, consider opting for spinal anesthesia and consult your healthcare provider to decide whether it suits your situation.






![13 Top Anesthesia Side Effects & Potential Risks [covered]](http://drnumb.com/cdn/shop/articles/shutterstock_1781191736_1.jpg?v=1693284851)

